At CodeToolz, our team utilizes a six-step process to provide support throughout the entire contract review process. From reviewing your contracts, to developing a negotiation strategy, our team of experts are here to make sure you get paid what you should.
6 Step Payer Contract Analysis
- Economic Testing
- Payer Matrix Development
- Score Matrix Against Economic Testing
- Develop Negotiation Strategy
- Negotiate Contract
- Update Matrix and Economic Testing
Improvement and change can be difficult to incorporate into the daily operations of physician practices. Factors such as decreases in reimbursement (due to Medicare and Medicaid funding cuts), increases in the uninsured population, declines in margins, and pressures from managed care organizations demand process improvements in the revenue cycle.
From large single and multi-specialty practice groups to hospital-employed physicians, we have helped hundreds of physicians make better business decisions. With managed care contracting services that are tailored to meet the needs of your practice, we look at every aspect of your payer contracts for ways to improve your payer reimbursements.
In the ever-changing healthcare landscape, you need a firm that can not only solve the complex problems of today but can also help you plan and innovate for the future. At CodeToolz, we do just that.
Because payer contracting is a tedious process that requires many-many steps and then multiple follow-up steps; our experts in the field take it on for you. They know how to engage with payers who are often more open to mutually beneficial reimbursement negotiations than you might imagine.
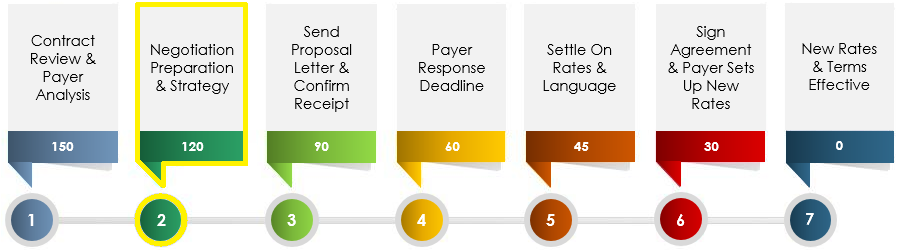
Payer Contract Negotiation Timeline (based on 150 days from Anniversary Date)